Yesterday when I tried to explain to a friend how Connor was dealing on his first day home after his first hospitalization for the BMT – he’s not in a good mood, but he’s not upset or agitated either – she said “so he’s just kind of resigned to it?” That’s exactly the word to use. He’s resigned to his fate and, like us, just dealing with things as they come.
But let’s back up a few days. Connor went into the hospital on Monday morning happy and cheerful. Almost immediately that changed when they had to draw blood and put in an IV. This took two nurses, a child life specialist, a psychologist, and both parents to hold him in place, distract him, console him, and reward him. He was pissed at all of us.
To calm him down afterwards I offered to draw him some pictures. I don’t know why this is one of his favorite activities, but it is. He instructs me on what to draw and I do my best to recreate it (keeping in mind that I haven’t taken a drawing class ever in my life and for my required applied arts classes in college I went with photography and sculpture). Until recently, he mostly wanted me to draw clues from Blues Clues, which is easy enough because Steve very nicely shows us how to draw them and isn’t a great artist himself. But now he’s getting more elaborate. He wants me to draw characters from Disney’s Robin Hood (his favorite movie at the moment) and Charlie Brown. And he wants them to look EXACTLY like the stills from the animations when he pauses the movies.
This activity kept him entertained in the oncology clinic, two OR waiting rooms, and the OR prep room (or whatever you call it where they bring you back and eight different people come in and ask you the same questions over and over and over and then you wait and wait some more until the anesthesiologist, who was one of those eight people, comes back and shoots you full of something to knock you out in ten seconds). For four hours I did nothing but create drawings on demand. We started with simple one-color characters and by the end I was drawing full color complete scenes and Connor wouldn’t let me stop until I drew in the curtains AND the trees.

That was the last time we saw Connor really happy. Since then it’s just been resigned.
So the surgery went well, but didn’t go as we had hoped. The original plan was to insert Connor’s Hickman line in such a way that it would come out by his shoulder, making it more difficult for him to be bothered by it and harder for him to access it and yank at it. Given how much he hates anything attached to his body, this was a real concern and we had a lot of discussions with his doctors about this. But when we got to the OR, there was some confusion–the people there thought they were inserting a Port-a-Cath, which gets implanted under the skin. There would be less to yank at, but would need to be accessed with needles (if I understand correctly, which is doubtful since I hadn’t heard this plan until just before the surgery so all of my knowledge comes from Googling it on my phone in the OR waiting room!). So not ideal, but it might be less annoying to Connor than a permanent floppy line. We agreed to this and Connor went off to surgery.
Five minutes later we were called back to the OR waiting room–the surgeon had concluded that he wouldn’t be able to tunnel the Hickman line out the back. What? We thought he was getting a Port-a-Cath! But no, we were right all along–Connor was getting a Hickman line and now we were being told that we’d just have to deal with multiple floppy lines coming out of his chest.
But in spite of all of this, the surgery went well. The moment of truth was when he woke up and got a look at the surgeon’s handiwork. Would he immediately start scrabbling at the tubes trying to get them off his body? While we waited in recovery, the nurses stood by with suggestions and called in an OT for further suggestions. Connor woke up and immediately starting clawing at…..his clothes. He wanted the stupid hospital gown OFF (there was some subterfuge involved here, I have to confess. Before his surgery we changed him into the hospital gown, he took it off and put his own clothes back on. We tried again right before his surgery and he fought back. So we knocked him out and let the surgical team change his clothes while he was asleep. It’s no wonder he wanted that gown off.). Once naked, Connor was much calmer. He was even more content when they removed his IV and the sticky sensors attached to his body. He wasn’t really pleased with the tape over the stitches put in at his neck where they accessed the vein for the Hickman line. But he left the central line and his g-tube alone.
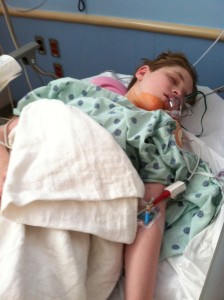
Then it was up to his room on the 11th floor while still groggy, where we’d wait for the chemo to begin.
A note about the rooms in the new children’s hospital at Hopkins: OK, so they are hospital rooms, which are never fun, but this building is gorgeous and the inpatient rooms are really nice. Lots of space (for a hospital room) and storage. The parent sleeping situation isn’t perfect (our room only had a lazy-boy type of chair; most rooms have a pull-out sofa thing that is far more comfortable). But what really makes the room is the view–we had a corner room with huge windows overlooking east Baltimore and the waterfront. East Baltimore, btw, looks a lot more picturesque from 11 floors up! Once Connor was up and moving (that wouldn’t happen until day 2) he spent a lot of time sitting in the recliner just looking out the windows.

I’m going to end this post here and save the other two days and his chemo for another post. Imagine me being too wordy when I write! 😉


